Overview
Whose ounce of prevention is worth the pound of cure? With the Total Patient Cost report you can compare agencies by the average Medicare spend for patients in the three months, six months, or year following a home health admission. Lower average overall costs indicate that an agency’s service is bending the cost curve for patients. Sometimes creating a better long-term outcome requires a bigger upfront investment!
![]() Using this information, you can improve your impact on the cost of providing care for a patient population and position yourself as a compelling partner for health systems that are focused on reducing overall costs within their patient population.
Using this information, you can improve your impact on the cost of providing care for a patient population and position yourself as a compelling partner for health systems that are focused on reducing overall costs within their patient population.
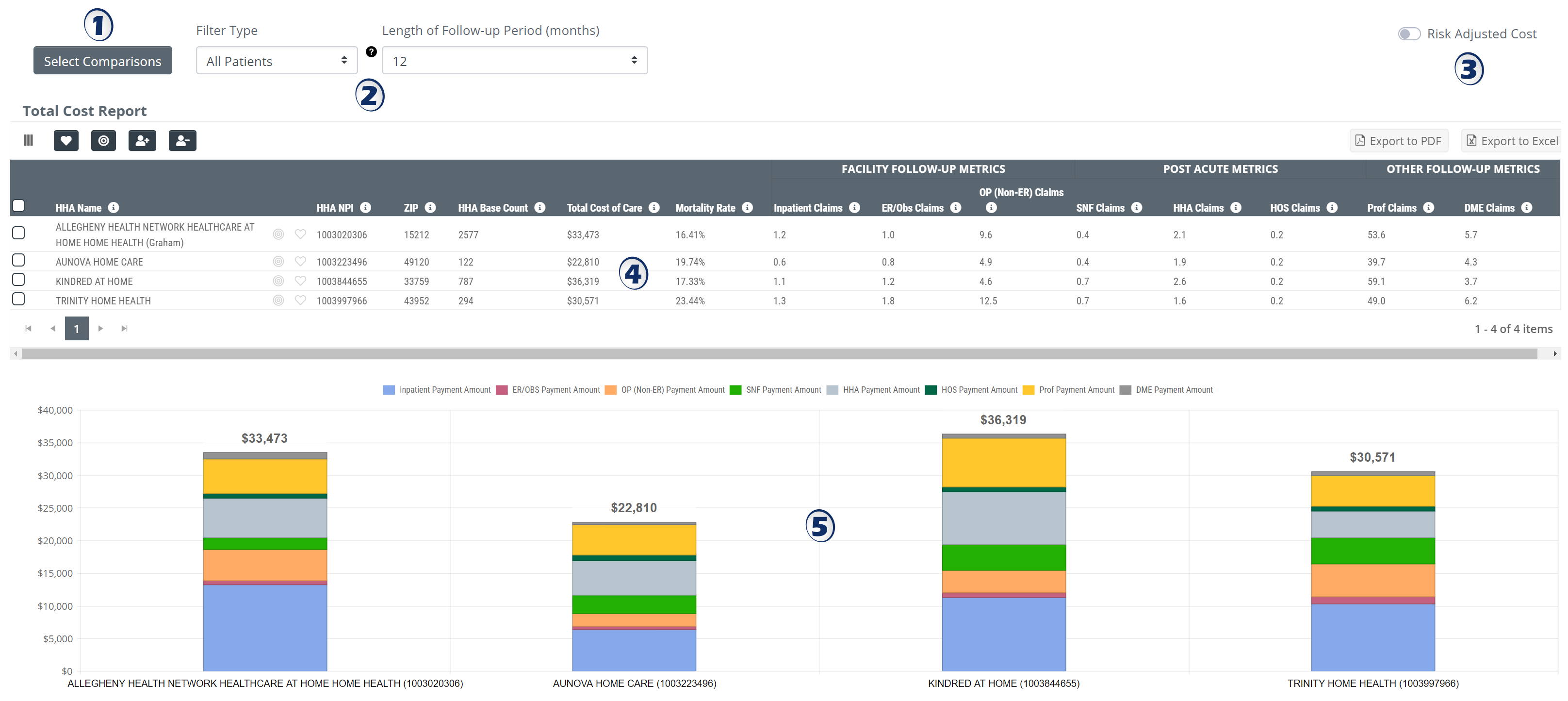
This report page includes a table and a graph that contain average Medicare expenditures for patients receiving treatment by the home health agencies that you select for examination. You can view these averages for a 3 month, 6 month or 12 month period aligned with the start of care for the home health agency. In addition, you can limit which claims data are used to calculate the averages by patient acuity, age, or by specific Trella Health Diagnostic Group.
Steps to use this Page
 Select Comparisons - required setup
Select Comparisons - required setup
When you click on the ![]() button, you will be able to add up to 7 Home Health agencies to the table and chart for comparison. The following interface will open when you click the button:
button, you will be able to add up to 7 Home Health agencies to the table and chart for comparison. The following interface will open when you click the button:
 Usage
Usage
- The Search field will allow you to enter a home health agency name or NPI to find it quickly.
- If you have selected favorite agencies, you can find them by clicking Favorites in the list on the left.
- User Home Health Agencies - will include every agency to which you have access.
- Once you have populated the Search Results field on the right, you can click on an agency to add it to your Selected Comparison(s). The agencies you add to the Selected Comparison(s) field will appear in the report table and chart.
![]() Best Practice - make sure you add your own agency to Selected Comparison(s) in order to compare your performance against your competitors.
Best Practice - make sure you add your own agency to Selected Comparison(s) in order to compare your performance against your competitors.
 Filters
Filters
You can focus the content of the table and chart using the filters.
![]() The filters are a powerful tool for evaluation. If a single agency is the most expensive, or the least, you can choose different filters to find out why. Choose an age filter to see who is spending the most on the oldest and therefore, most acute patients. Or examine different diagnoses to identify who is treating the most difficult patients, who might cost more.
The filters are a powerful tool for evaluation. If a single agency is the most expensive, or the least, you can choose different filters to find out why. Choose an age filter to see who is spending the most on the oldest and therefore, most acute patients. Or examine different diagnoses to identify who is treating the most difficult patients, who might cost more.
![]() When you choose Acuity, Age, or MDC, an additional filter option will open to allow additional refinement of the chosen filter type. The options in the new filter, Filter Selection, are shown below.
When you choose Acuity, Age, or MDC, an additional filter option will open to allow additional refinement of the chosen filter type. The options in the new filter, Filter Selection, are shown below.
Filter Type
This allows you to choose different sets of patients for which the metrics on the page will be calculated:
| Filter Type | Filter Selection Options |
| All Patients | Every patient treated by the agency/agencies will be included in the metrics |
| Acuity |
Allows you to select High, Medium or Low acuity patients:
|
| Age |
Choosing an age category allows you to limit the metrics to patients who are younger than 65, 65 to 74, 75 to 84, or 85 and older.
|
| Trella Health Diagnostic Grouping |
The Trella Diagnostic Group filter Selection allows you to limit metrics to patients in one of the Trella Health Diagnostic groups.
For more information view Trella Health Diagnostic Groupings. |
Length of Follow up Period
With this filter you can change the period from which we gather expenses to be added to the report. The time periods begin at the time of home health start of care and you can select a 3-month, six-month, or 12-month period as the follow-up period.
In order to provide the necessary period of time from Admission to the end of the most recent quarter of data, we offset the one year reporting period to provide a full year of admissions.
![]() Although the three month follow up period is not shown in this image, it follows the same pattern.
Although the three month follow up period is not shown in this image, it follows the same pattern.
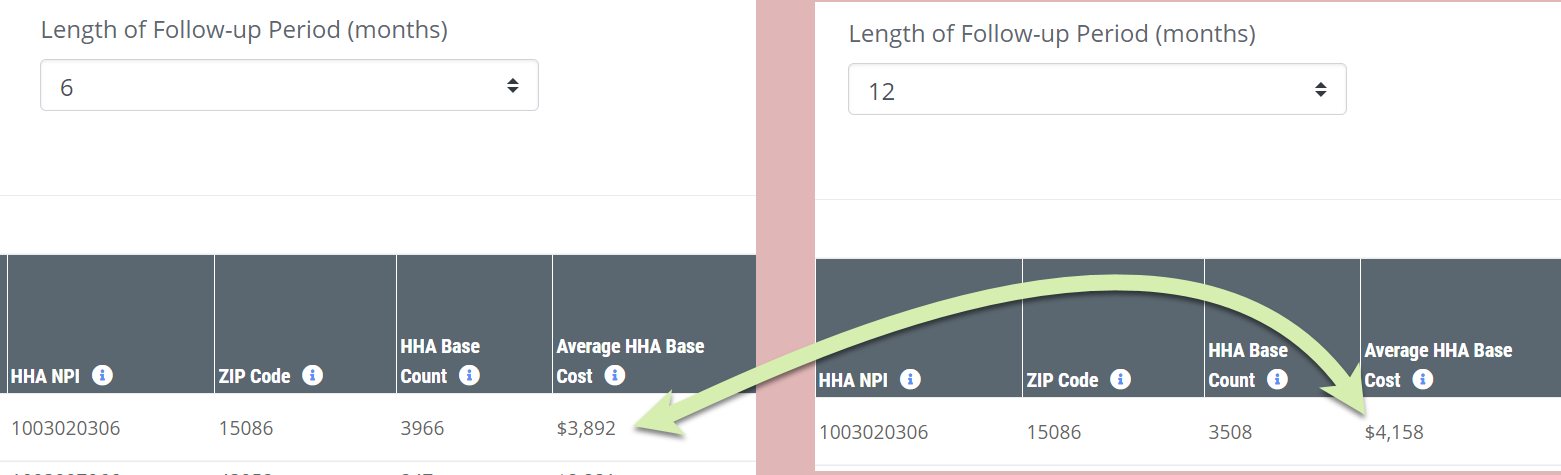
Why does the base cost change?
When you change from one follow up period to another, you will notice that the HHA Base Count and the Average HHA Base Cost change. (See image.)
In general, the patients in a pool (cohort) used for calculations are identical when a metric is calculated from the same one-year reporting period. An example of this would be a population of patients defined as "all patients admitted to home health care during the one year reporting period." As it is, that is one of the specifications for the base count and average base costs metrics under consideration.
The added parameter in the case of these "base" metrics is the follow-up period restrictions. For these metrics, for a patient to be counted, they must be a beneficiary of Medicare services throughout the entire calculation period, from the start of care throughout the entire follow up period.
We do this so that follow up costs are comparable, that is, we only include patients in these metric who received services, and incurred costs, through the entire period.
A patient who went off service before completing the entire follow up period would pull the average down as a result of having less cost-related care.
Whether the loss of service is caused by a death or loss of coverage, it is highly likely that more patients will lose coverage during a longer (12-month) period than a shorter (6-month) period.
 Risk Adjusted Cost
Risk Adjusted Cost
Clicking this toggle ![]() will adjust the metrics on the page to present a risk-adjusted version of the table and chart. Since higher patient risk scores indicate a population with more severe medical conditions, adjusting the cost based on population severity allows for a more comparable cost analysis among home health agencies.
will adjust the metrics on the page to present a risk-adjusted version of the table and chart. Since higher patient risk scores indicate a population with more severe medical conditions, adjusting the cost based on population severity allows for a more comparable cost analysis among home health agencies.
The HCC risk scores are used to adjust cost relative to other NPIs of the same provider type. Adjusted costs allow for better comparison across NPIs with different risk scores because it accounts for the increased cost of patients with chronic conditions. For example, NPIs with a higher than average risk score will have a reduced adjusted cost since they have sicker patients, and NPIs with lower risk scores have increased adjusted cost.
For more information on Risk Scores - ![]()
 Total Cost Table
Total Cost Table
This table contains the key metrics for the selected agencies. Examine the chart below
![]() Follow-Up in this table is not a reference to subsequent care, it is a reference to the different periods of time you can select to apply as the length of time during which the table includes expenses after the start of care.
Follow-Up in this table is not a reference to subsequent care, it is a reference to the different periods of time you can select to apply as the length of time during which the table includes expenses after the start of care.
| Metric | Descriptions | |
| Agency | Agency Name, NPI and ZIP Code | Home health agency name, NPI, and ZIP code for the listed agency, as listed in the CMS Provider Data (NPI) file. |
| HHA Base Count |
This is the count of home health stays from which the metrics are calculated.
|
|
| Total Cost of Care |
This is the average Medicare spend (both Part A and Part B) for the selected stays.
|
|
| Mortality Rate | The percentage of the HHA Base count patients who died during the selected follow up period. | |
|
Facility Follow-Up Metrics Averages |
Inpatient Claims | This is the average count of inpatient claims submitted during the selected follow-up period. (Includes LTACH and IRF.) |
| ER/OBS Claims | The average count of emergency room and outpatient observation claims submitted during the selected follow up period. | |
| OP (Non-ER) Claims | This metric is the average count of non emergency room or observational claims submitted during the selected follow-up period. | |
|
Post Acute Averages |
SNF Claims | The average count of skilled nursing claims submitted during the selected follow-up period. |
| HHA Claims | The average count of home health claims submitted during the selected follow-up period. | |
| HOS Claims | The average count of hospice claims submitted during the selected follow-up period. | |
| Other | Prof Claims | The average count of professional claims submitted during the selected follow-up period. Professional claims are "carrier" claims submitted by professional providers, including physicians, physician assistants, clinical social workers, nurse practitioners. |
| DME | The average count of durable medical claims submitted during the selected follow-up period. | |
 Comparison Chart
Comparison Chart
The report includes an interactive chart. Hovering over a bar in the graph shows the Medicare spend broken out by claim type.

![]() Clicking on any of the elements in the legend will turn that claim type off or on in the chart. By using this feature, you can have one, some, or all claim types shown, in any combination.
Clicking on any of the elements in the legend will turn that claim type off or on in the chart. By using this feature, you can have one, some, or all claim types shown, in any combination.
FAQ - HHA Base Cost vs. HHA Payment Amount
If you look at the following image notice that the two metrics are not the same. Why not? They both seem to be average costs for home health services.
That is true, they are both metrics for home health services. The top average ($4,158) is the average cost for the initial home health stay. The lower cost ($6,390) is the total patient cost for home health services from the start of care for the original stay and any additional home health costs subsequent to the initial stay during the chosen follow-up period.
As you can see from the image below, the top metric only includes costs for the "Home Health Stay" after the HHA Start of Care (SOC). Any additional costs that occur during the follow up period will be added to the average.